 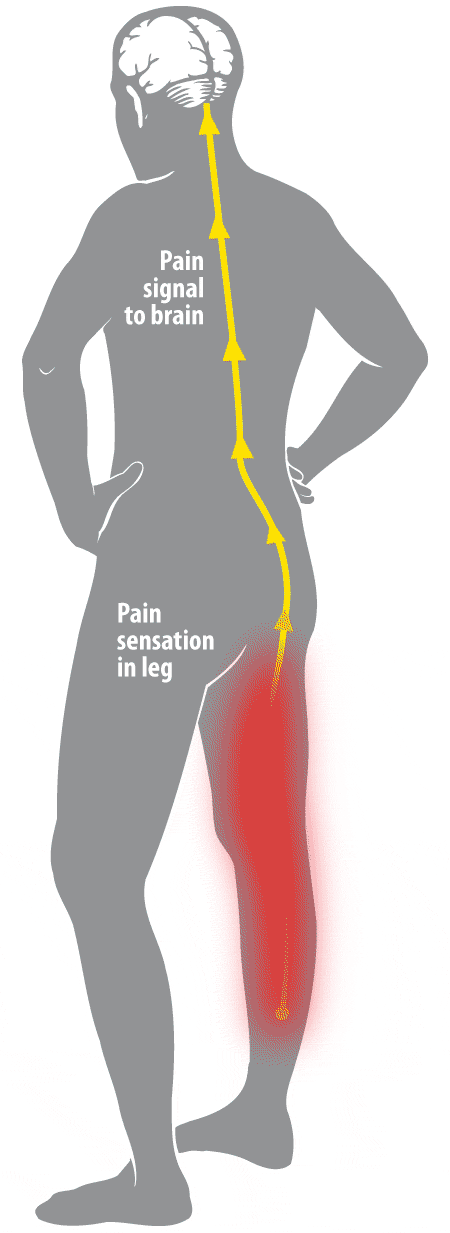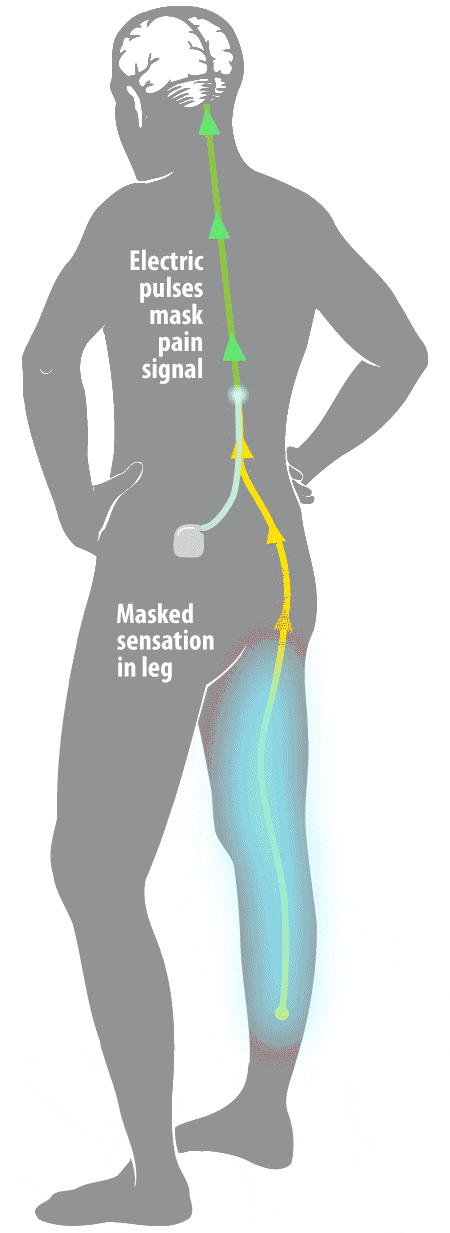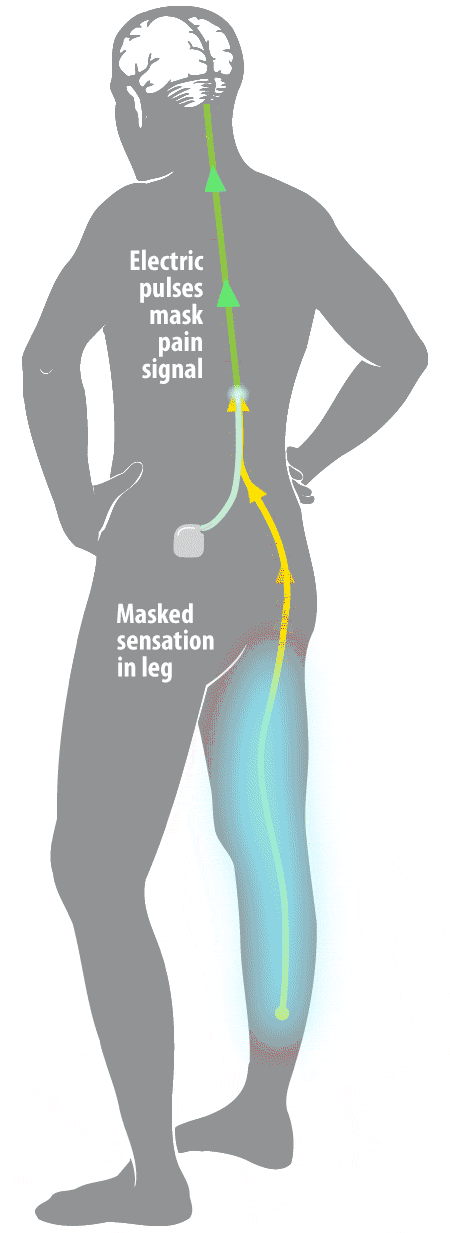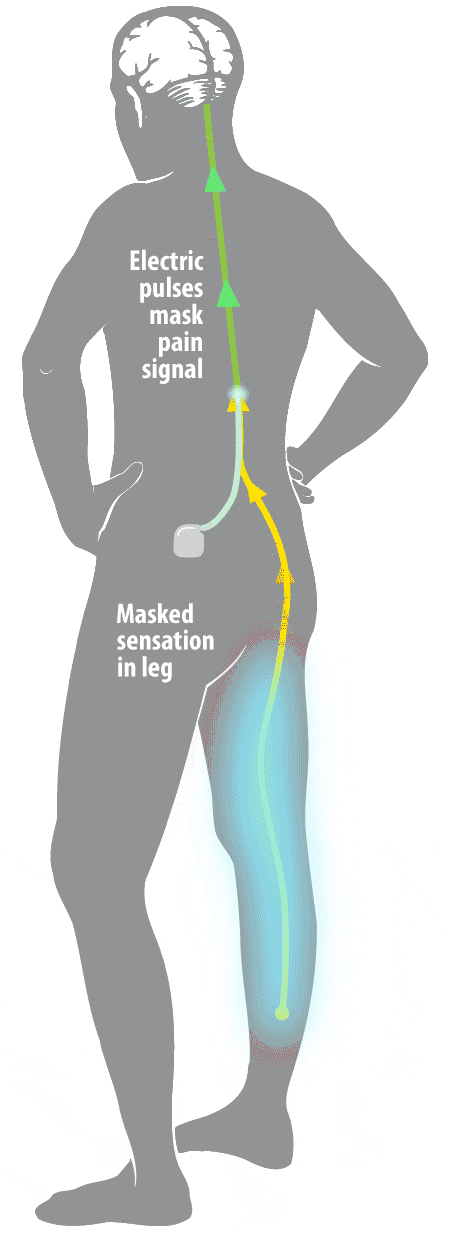  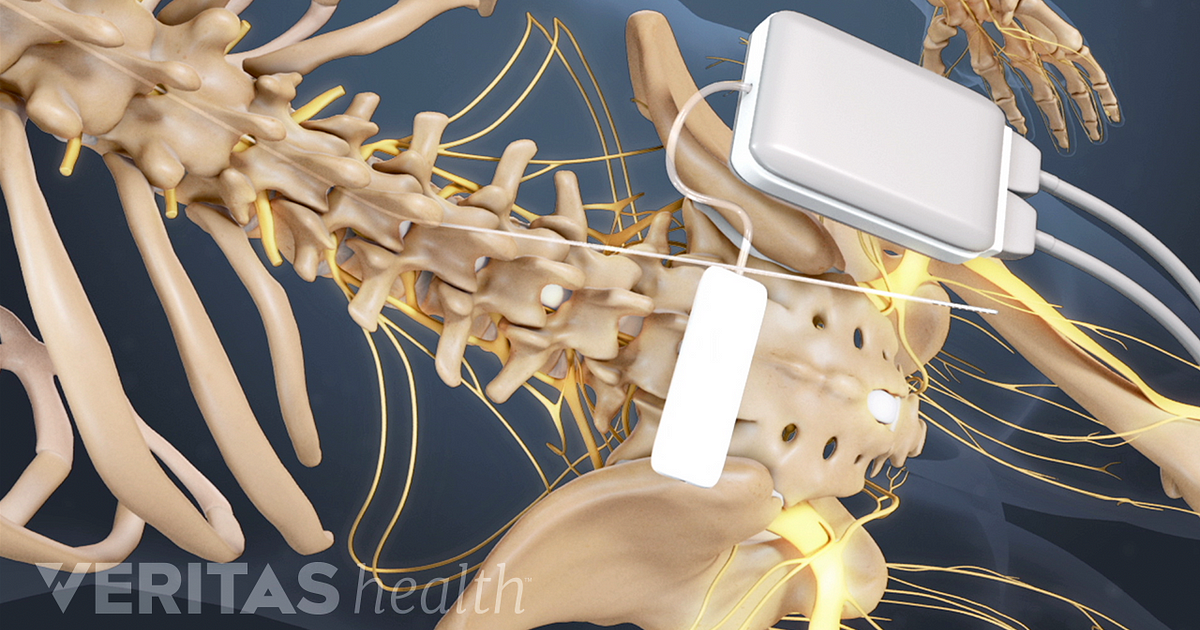
Studies of SCS have shown that the therapy significantly improves the health-related quality of life (HRQoL) of users. Despite incomplete understanding of the mechanism of action, spinal cord stimulation (SCS) has become increasingly popular and its efficacy has been documented in neuropathic pain (level B) as well as ischemic pain, whether due to peripheral vascular or coronary artery disease. The electrical stimulation of the dorsal columns of the spinal cord to induce pain relief was first used in humans in 1967. Serious adverse events such as neurological damage are rare. Hardware-related complications are more commonly observed than biological complications. Spinal cord and peripheral neurostimulation techniques are safe and reversible therapies. Serious biological complications such as dural puncture headache and neurological damage are rarely observed.Ĭonclusions. Common biological complications include infection and pain over the implant. Other lead related complications such as failure or fracture have also been reported. The commonest hardware-related complication is lead migration. Adverse events can be subdivided into hardware-related complications and biological complications. The incidence of complications reported varies from 30% to 40% of patients affected by one or more complications. A review of the major recent publications in the literature on the subjects of spinal cord, occipital, sacral, and peripheral nerve field stimulation was conducted. The aim of this article is to present a review of complications observed in patients treated with neurostimulation techniques. Neuromodulation has recognized complications, although very rarely do these cause long-term morbidity. Spinal cord and peripheral neurostimulation techniques have been practiced since 1967 for the relief of pain, and some techniques are also used for improvement in organ function. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
